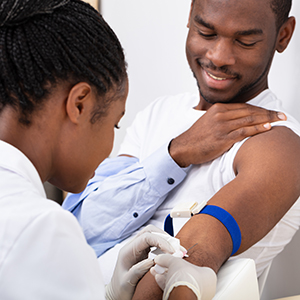
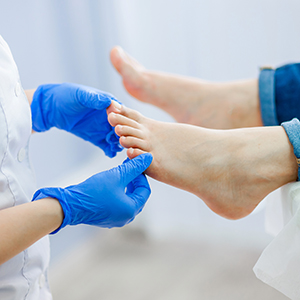
Care Schedule and Screenings
Diabetes is a chronic (long-term) condition, but you can still lead a healthy and active lifestyle with the right steps – like making regular visits to your healthcare provider and creating daily routines. Below is the recommended care schedule, including screenings, appointments, and lifestyle modifications, help keep you healthy and getting the care you need.
Three important screenings to prioritize:
Diabetes is a challenging condition, but you can keep your symptoms in check by sticking to a routine schedule both daily and throughout the year. Work with your healthcare provider to set up a care schedule or make a commitment to stick your plan if you already have one.
Looking for more tips and education? Click the button below to team up with a diabetes educator or join a support group.
Team up with a Diabetes Care and Education Specialist

Living with diabetes can be overwhelming. Let us help. Get expert advice and support with Text for Tips. Simply opt-in using this quick and easy form to receive weekly guidance, diabetes-friendly recipes, motivational messages, and more.